MobileLink


Many years of experience with successful implant systems and a range of fixation concepts, together with state-of-the-art material and coating technologies, have gone into the development of this new acetabular cup system. The result is the versatile cementless MobileLink Acetabular Cup System.
The MobileLink Acetabular Cup System comes in two different versions: A cluster-hole press-fit cup and a multi-hole press-fit cup. Both versions of the shells are available in a PlasmaLink, a TiCaP double coating or a TrabecuLink surface.
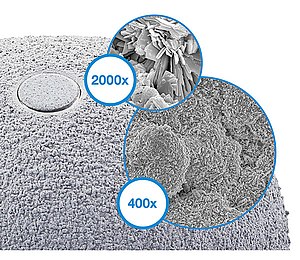
The TiCap double coating combines a porous surface for primary fixation with our osteoconductive2 HX calcium phosphate coating. This combination is designed to give optimal primary stability and osseointegration.
The 3-dimensional TrabecuLink structure, with its pore size, porosity and structure depth, also provides an excellent basis for promoting osteoconduction and microvascularization, taking into account the requirements for the structure-covering protein layer (fibronectin - vitronectin - fibrinogen).4,5

The MobileLink Acetabular Cup System can be used with ceramic or UHMWPE inserts. UHMWPE inserts are available in X-LINKed and E-DUR (X-LINKed, Vit-E PE) versions. All UHMWPE inserts are available in a standard version and also with protection against luxation. The MobileLink Acetabular Cup System can be combined with modular offset and/or inclining casing/insert adapters (Face Changer). The adapters allow restoration of the anatomy in revision cases. In addition, the adapters permit the use of ceramic inserts in revision arthroplasties.

The MobileLink Acetabular Cup System can be transformed into a modular dual mobility system, with the use of Dual Mobility Inserts made from EndoDur. The DM insert is to accommodate poly DM liners from the BiMobile Dual Mobility System.
The Dual Mobility concept was developed by Prof. Gilles Bousquet in the 1970s with the aim of avoiding recurrent hip luxations. A modular Dual Mobility System is composed of a Dual Mobility Insert with a highly polished inner surface placed in a Shell in which a mobile polyethylene liner having a pressed in prosthesis head is moving.
Features and Advantages of Dual Mobility:
- Dual mobility leads to reduced risk of dislocation and increased range of motion (RoM) 6
- Polished inner surface for minimized wear and a prolonged implant life 7,8
- Self-centering Liner promotes even wear patterns and enhances dislocation resistance 9


The 3-dimensional TrabecuLink structure, with its pore geometry (porosity: 70%, pore size: 610-820 μm, structure depth: up to 1 mm) ensures excellent cell ongrowth. 4,5,10
Pore filling
The sequence of images shows a pore of the TrabecuLink structure being filled with tissue under in-vitro cell culture conditions. The fibronectin laid down by human fibroblasts and continually reorganized over a period of eight days is visible as green fibers. Fibronectin is a component of the extracellular matrix that is formed at an early stage of the healing process. It forms a basis for the embedding of collagen, which is essential for mineralization of the tissue and ingrowth of bone into the structure. Apart from the accumulation of fibronectin, which increases over time, a clear contraction of the matrix towards the center of the pore can be observed. This contraction mechanism, which is attributable to the cellular forces acting in the tissue, accelerates the rate at which the pore is filled with tissue, compared to a layer-by-layer tissue growth (Reference: Joly P et al., PLOS One 2013; journals.plos.org/plosone/article. Julius Wolff Institute, Charité - Universitätsmedizin Berlin
Features and advantages
Wide choice of sizes (Ø 42-80 mm)
Choice of latest materials, such as E-DUR® Polyethylene
Clinically proven rough TiCaP® Double Coating 2
Secure – triple fixated inserts
Unique technology of the Face Changer fixation1,3
50/36 mm – small outside, large inside
Color coding for efficient work flow
High flexibility, minimal stock holding
Intraoperative flexibility
Simple instrument set and color coding for efficient surgical procedures
Casing/insert adapter (Face Changer) for anatomical reconstruction1
Variable options for placing bone screws 1
- Data on File, Waldemar Link.
- Ullmark G, Sorensen J, Nilsson O. Analysis of bone formation on porous and calcium phosphate-coated acetabular cups: a randomised clinical [18F]fluoride PET study. Hip international: the journal of clinical and experimental research on hip pathology and therapy. 2012;22(2):172-8.
- PCT-Patent Application WO 2017/140497 A1
- Cecile M. Bidan, Krishna P. Kommareddy, Monika Rumpler, Philip Kollmannsberger, Yves J.M. Brechet, Peter Fratzl, John W.C. Dunlop. et al.; How Linear Tension Converts to Curvature: Geometric Control of Bone Tissue Growth; PLoS ONE 7(5): e36336. doi.org/10.1371/journal.pone.0036336 (2012)
- Pascal Joly, Georg N. Duda, Martin Schöne, Petra B. Welzel, Uwe Freudenberg, Carsten Werner, Ansgar Petersen, et al.; Geometry-Driven Cell Organization Determines Tissue Growth in Scaffold Pores: Consequences for Fibronectin Organization; PLoS ONE 8(9): e73545. doi.org/10.1371/journal.pone.0073545 (2013)
- Stroh, D. Alex, et al. "Dual-mobility bearings: a review of the literature." Expert review of medical devices 9.1 (2012): 23-31.
- Long, M., & Rack, H. (1998). Titanium alloys in total joint replacement—a materials science perspective. Biomaterials, 19(18), 1621-1639
- Loving L, Herrera L, Banerjee S, Heffernan C, Nevelos J, Markel DC, Mont MA. 2015. Dual mobility beari ngs withstand loading from steeper cup-inclinations without substantial wear. J Orthop Res. 33(3):398-404.
- Fabry C, Kaehler M, Hermann S, Woernle C, Bader R. 2014. Dynamic behavior of tripolar hip endoprostheses under physiological conditions and their effect on stability. Medical Engineering & Physics 36:65– 71.
- Steinemann SG; Compatibility of Titanium in Soft and Hard Tissue – The Ultimate is Osseointegration; Materials for Medical Engineering, WILEY-VCH, Volume 2, Page 199-203












